|
6/19/2023 0 Comments Brisk capillary refills
Choose a digit without nail polish and anything that could restrict blood flow to the area, such as jewelry or a watch. Greet the patient, explain the procedure, and obtain consent.ģ. Before performing any nursing skills or assessments, it is important to verify the latest protocols for your facility, as nursing skills and assessment criteria may change over time.Ģ. Note: This information is for educational purposes only. Here are some tips to perform the capillary refill test on a patient’s fingernail or pad of finger. How to Perform a Capillary Refill Test on a Fingernail Colder temperatures (either the patient’s body or room temperature).In addition, some of the factors below may affect the reliability of the capillary refill test or lead to longer than normal capillary refill time: Raynaud’s disease: this can cause vessels to spasm and/or narrow in extremities that are exposed to cold, which reduces blood flow.Peripheral vascular disease: In peripheral vascular disease, the narrowing of vessels can reduce tissue perfusion.Cast care and placement: If a cast is placed on a broken limb, capillary refill time is often assessed to ensure that proper blood flow is reaching the extremity and that the cast is not too tight.Bone fractures: compartment syndrome may develop during a fracture, which can restrict blood flow in the affected limb.Decreased cardiac output: This may be due to shock, heart failure, anemia, and other similar conditions.Some examples of factors that can cause poor peripheral perfusion include the following: What Causes an Abnormal Capillary Refill Time?Ī capillary refill test of longer than 2 or 3 seconds could indicate that the patient is experiencing poor peripheral perfusion (blood flow to the extremities) or even dehydration. Note: Some guidelines or studies suggest that a capillary refill of up to three seconds could be normal in some patient populations, so always refer to your facility’s protocols for details. If the blood flow returns to the tissue within 2 seconds (depending on your facility’s protocols), it is considered a normal finding, but longer than 2 seconds could be considered abnormal and should be reported immediately. Note: The capillary refill test may sometimes be performed on the sternum or forehead in some patient populations, such as newborns. The nurse then releases the digit and observes the number of seconds it takes for the tissue to regain its natural color as blood flow resumes. Nurses typically perform the capillary refill test by pressing on the nail plate or the pad of a digit for around 5-10 seconds, causing the nail bed (or pad of digit) to lighten in color as the blood is expelled. Post Peer Reviewed By: Salim R.How is the Capillary Refill Test Performed? Neurogenic:↓ sympathetic output, and may have bradycardia due to unopposed vagal toneīasics of Shock – Educational Reinforcement Materialīasics of Shock – Supplemental Educational Material.Hepatic failure: ↑ endogenous Nitric Oxide which is a potent vasodilator.Adrenal Insufficiency:↓Cortisol (up-regulates vascular tone ↓ catecholamine release).Sepsis: Sepsis is unique and patients have components of hypovolemic shock and cardiogenic shock (Myocardial depression from circulating cytokines). 
Warm Shock:↓Systemic vascular Resistance (ie Vasodilatory Shock)Ĭategories of Warm Shock: Just 1 Distributive Shock, but 5 main causes of Distributive Shock ↓peripheral pulses (later stages,↓ central pulses).Narrow Pulse Pressure (compensation by vasoconstriction and ↑SVR).Systolic Blood Pressure correlates with stroke volumeĭeterminants of SV: Preload, Contractility, and Afterload Lactate elevation doesn’t always mean a patient is in shock or has sepsis (although lactate is elevated in these conditions), but you must have a broad differential as lactate can be elevated for many additional reasons. Lactate is produced in shock under aerobic conditions due to B2 adrenergic stimulation from elevated epinephrine levels. Lactate: Usually elevated in shock, but the classic belief that lactate is elevated because of anaerobic metabolism and tissue hypoxia is not the main reason. 
Shock occurs when supply does not meet demands and NOT defined by a blood pressure (patients may be normotensive, or even hypertensive in shock) Also Be Sure to Checkout our YouTube Channel In this post, the basics of shock, we will define shock, discuss the causes of lactate elevation, and review the main categories of shock. Emphasis in defining shock is based on tissue perfusion in relation to cellular function. 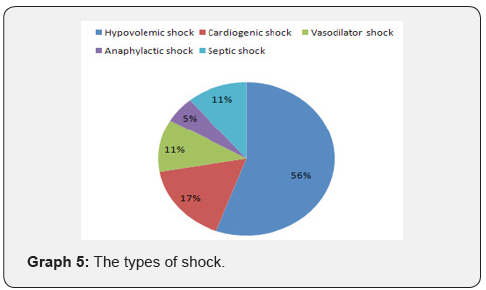
Assessment of perfusion is independent of arterial pressure, in that hypotension does not always need to be present to define shock. The magnitude of the problem is illustrated by the high mortality associated with shock. Shock is one of the most important problems with which physicians will contend with.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
